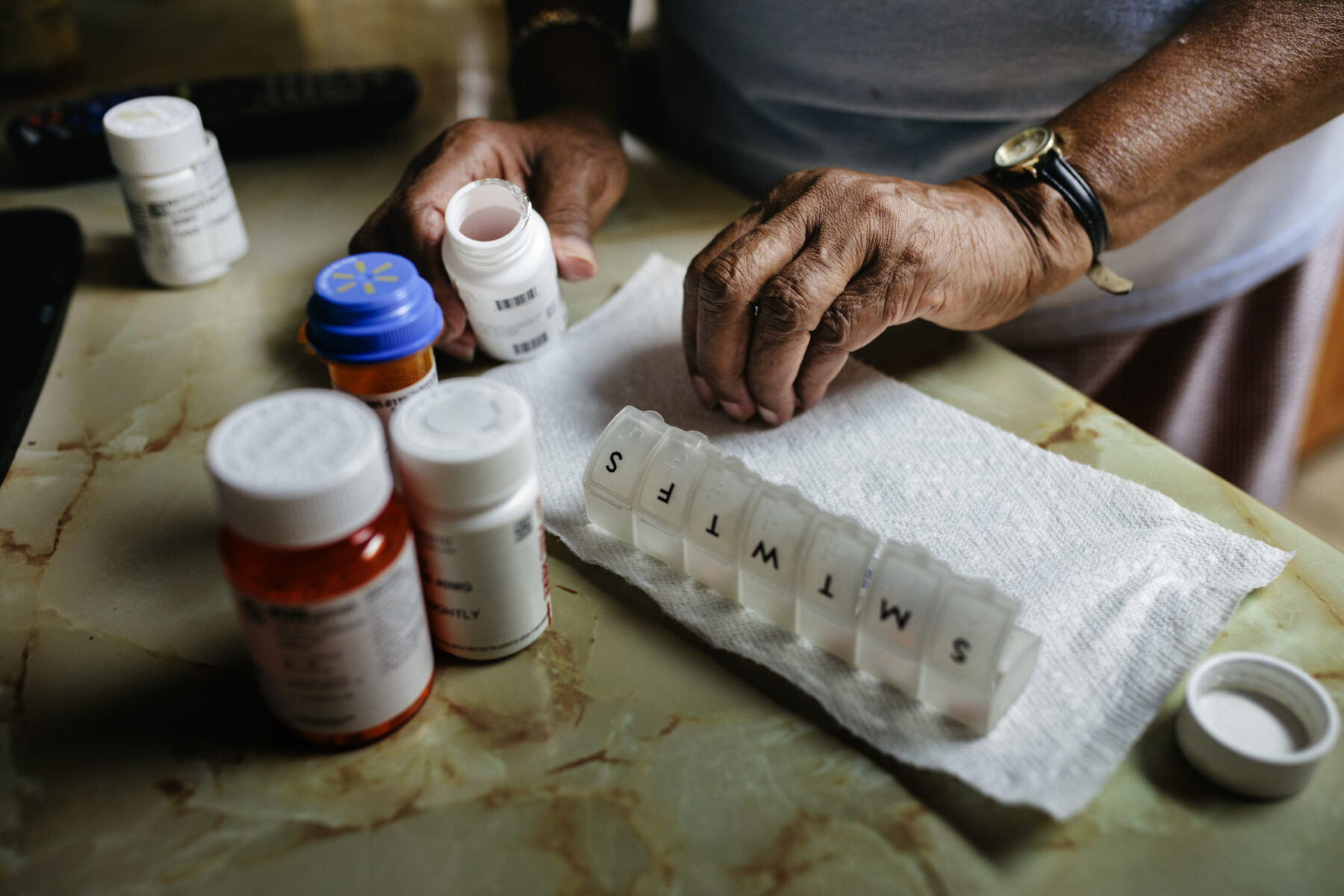
In an effort to fulfill campaign promises to lower prescription drug prices, President Biden recently signed an executive order aimed at strengthening competition in the pharmaceutical industry and allowing states to import less-expensive drugs from Canada.
The order itself doesn’t directly lower prices; instead, it directs federal agencies to intensify their efforts to address rising drug prices that have resulted, in part, from the proliferation of anticompetitive tactics — such as pay-for-delay deals and product-hopping — that have been embraced by big pharma to squeeze out competition and extract large profits.
These tactics have recently come under fire by the American public and by lawmakers, including the Senate Judiciary Subcommittee on Competition Policy, Antitrust and Consumer Rights, which recently held a hearing exposing manipulations by drug manufacturers to extend market exclusivity and raise prices.
Against this backdrop, Biden’s executive order aims to address rising drug prices by:
- Directing the Health and Human Services (HHS) to increase support for generic drugs and biosimilars, which are less expensive alternatives to brand name biologic drugs
- Directing HHS to issue a comprehensive plan to combat high prescription drug prices and price gouging
- Encouraging the Federal Trade Commission (FTC) to ban pay-for-delay deals — a tactic used by manufacturers to pay generic and biosimilar competitors to delay the launch of cheaper drugs — and similar anticompetitive agreements
- Directing the Food and Drug Administration (FDA) to work with states and tribe to safely import prescription drugs from Canada
We explain the ways in which the order, though it is a move in the right direction, falls short of its goal and how additional legislative steps are needed next to ensure more meaningful reform.
Strengthening competition
The order takes a positive step forward in advancing efforts to stop pharma’s use of tactics that impede competition for less-expensive generic and biosimilar drugs by encouraging the FTC to strengthen enforcement over such techniques. However, this alone will be unlikely to result in lower drug prices and tangible savings for taxpayers and consumers without more comprehensive legislative action.
Pay-for-delay settlements are often very difficult for the FTC to prosecute as they have become more cleverly disguised and can involve complex side-deals that are challenging to unravel. Between 2010 and 2015, the number of pay-for-delay settlements increased 50%. Yet, the FTC has challenged only a few in the last decade.
Even if the FTC strengthened its enforcement of pay-for-delay deals, manufacturers will continue to benefit from the extra weeks — or even months — of monopoly power from the arrangements, further incentivizing brand name drug makers to pursue these deals.
Effective solutions to end pay-for-delay must address both the generic and biosimilar markets — and attempt to contemplate newer generations of pay-for-delay settlements that may not involve direct payments. In addition, the penalties must be sufficiently strong to discourage the behavior in the future.
Lawmakers have introduced a bipartisan bill, Preserve Access to Affordable Generics and Biosimilars Act (H.R. 2375), that would require manufacturers to prove an agreement is not anticompetitive rather than asking the FTC to prove an agreement is anticompetitive. A version of this bill has been introduced in every Congress since 2005.
Improving the patent system
Pharma has also exploited the U.S. patent system to raise prices and thwart competition. While Biden’s executive order does not lay out specific policy solutions, it does acknowledge that the patent system is an area that has been subverted by the pharmaceutical industry to unjustifiably delay generic drug and biosimilar competition.
One way drug manufacturers game the patent system is by seeking weak, invalid patents. The Patent Trial and Appeal Board (PTAB) was established in 2012 with the goal of correcting these validity errors in a manner that is less expensive and more scientifically accurate than court litigation challenges. However, new research finds that the PTAB is not playing an active enough role in policing the validity of drug patents, and isn’t targeting patents of a particular quality.
Arti Rai, professor of law at the Duke University School of Law and an Arnold Ventures grantee, recently co-authored a paper detailing these findings and is recommending that policymakers consider revisiting statutes that create incentives to pursue district court litigation over PTAB when challenging certain drug patents.
Importing less-expensive drugs
Lastly, the order directs the FDA to continue a policy supported by the Trump Administration to help states and tribal nations safely import less-expensive prescription medications from Canada, but the directive faces significant hurdles and we do not believe it is a policy that can resolve drug pricing issues in the U.S.
Canada is one of many high-income countries that have used coordinated government negotiation to get access to drugs that are significantly cheaper than the same drugs in the United States. However, the Canadian pharmaceutical market is far too small to support importation to the U.S. With only one-tenth of the population of the U.S., importation at scale would require a massive increase in purchases from Canadian wholesalers. It is unlikely manufacturers would willingly go along with this understanding that increased order volume is just being repackaged for the U.S. market.
At least 10 states have advanced laws to import drugs from Canada – the lobbying group Pharmaceutical Research and Manufacturers of America (PhRMA) has sued in federal court to stop the laws. The Biden Administration has asked the court to dismiss the suit.
For more information about policies to lower drug prices, read our brief.