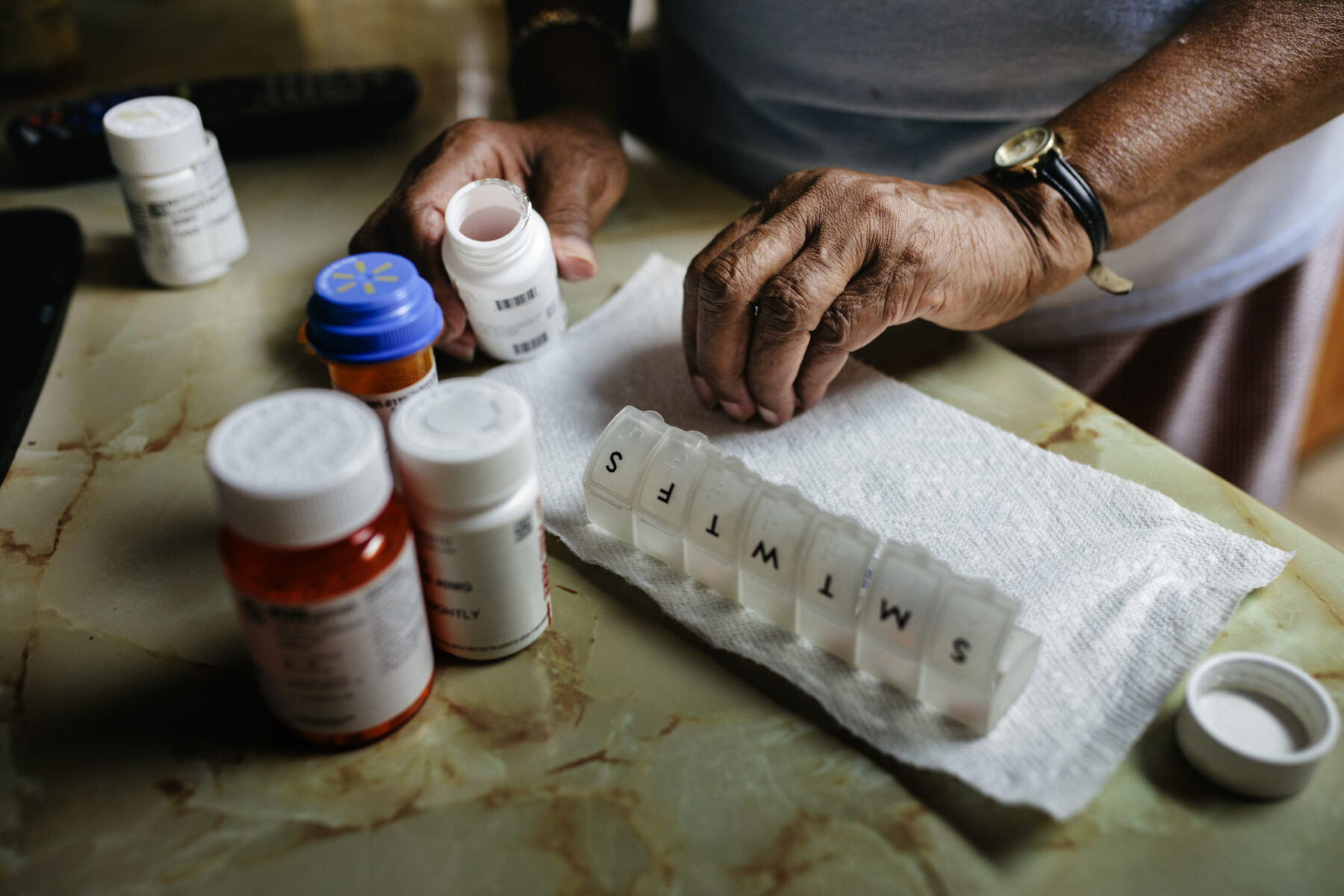
In 2011, Elsa Dixler was diagnosed with multiple myeloma. That August, she was prescribed Revlimid, a drug that had come on the market six years earlier. By January 2012, she went into full remission, where she has remained since. So long as Revlimid retains its effectiveness, she will take it for the rest of her life.
“I was able to go back to work, see my daughter receive her Ph.D, and have a pretty normal life,” said Dixler, a Brooklyn resident who is now 74. “So, on the one hand, I feel enormously grateful.”
But Dixler’s normal life has come at a steep financial cost to her family and to taxpayers. Revlimid typically costs nearly $800 per capsule, and Dixler takes one capsule per day for 21 days, then seven days off, and then resumes her daily dose, requiring 273 capsules a year. Since retiring from The New York Times at the end of 2017, she has been on Medicare. Dixler entered the Part D coverage gap (known as the donut hole) “within minutes,” she said. She estimates that adding her deductible, her copayment of $12,000, and what her Part D insurance provider pays totals approximately $197,500 a year.
Revlimid should have been subject to competition from generic drug makers starting in 2009, bringing down its cost by many orders of magnitude. But by obtaining 27 additional patents, eight orphan drug exclusivities and 91 total additional protections from the U.S. Food and Drug Administration (FDA) since Revlimid’s introduction in 2005, its manufacturer, Celgene, has extended the drug’s monopoly period by 18 years — through March 8, 2028.
“I cannot fathom the immorality of a business that relies on squeezing people with cancer,” Dixler said, noting her astonishment that Revlimid has obtained orphan drug protections when it treats a disease that is not rare and does not serve a very limited population. She also observed that Revlimid’s underlying drug is thalidomide, which has been around for decades. “They didn’t invent a new drug, rather, they found a new use for it,” she said.
“The cost of Revlimid has imposed constraints on our retirement,” Dixler said, “but when I hear other people’s stories, I feel very lucky. A lot of people have been devastated financially.”
Revlimid is a case study in a process known as “evergreening” — artificially sustaining a monopoly for years and even decades by manipulating intellectual property laws and regulations. Evergreening is most commonly used with blockbuster drugs generating the highest prices and profits. Of the roughly 100 best-selling drugs, more than 70 percent have extended their protection from competition at least once. More than half have extended the protection cliff multiple times.
The true scope and cost of evergreening has been brought into sharper focus by a groundbreaking, publicly available, comprehensive database released Thursday by the Center for Innovation at the University of California Hastings College of Law and supported by Arnold Ventures.
The Evergreen Drug Patent Search is the first database to exhaustively track the patent protections filed by pharmaceutical companies. Using data from 2005 to 2018 on brand-name drugs listed in the FDA’s Orange Book — a listing of relevant patents for brand name, small molecule drugs — it demonstrates the full extent of how evergreening has been used by Big Pharma to prolong patents and delay the entry of generic, lower-cost competition.
“Competition is the backbone of the U.S. economy,” said Professor Robin Feldman, Director of the UC Hastings Center for Innovation, who spearheaded the database’s creation. “But it’s not what we’re seeing in the drug industry.
“With evergreening, pharmaceutical companies repeatedly make slight, often trivial, modifications to drugs, dosage levels, delivery systems or other aspects to obtain new protections,” she said. “They pile these protections on over and over again — so often that 78 percent of the drugs associated with new patents were not new drugs coming on the market, but existing drugs.”
Competition is the backbone of the U.S. economy. But it’s not what we’re seeing in the drug industry.Professor Robin Feldman Director of the UC Hastings Center for Innovation
In recent decades, evergreening has systematically undermined the Drug Price Competition and Patent Term Restoration Act of 1984, which created the generic drug industry. Commonly known as the Hatch-Waxman Act, it established a new patent and market exclusivity régime in which new drugs are protected from competition for a specified period of time sufficient to allow manufacturers to recoup their investments and earn a reasonable profit. When that protection expires, generic drug makers are incentivized to enter the market through a streamlined regulatory and judicial process. Drug prices typically drop by as much as 20 percent when the first generic enters the market, and with more than one generic manufacturer, prices can plummet by 80 to 85 percent.
“Hatch-Waxman created an innovation/reward/competition cycle, but it’s been distorted into an innovation/reward/more reward cycle,” Feldman said. “To paraphrase something a former FDA commissioner once said, the greatest creativity in Big Pharma should come from the research and development departments, not from the legal and marketing departments.”
Feldman led the development of the Evergreen Drug Patent Search in response to repeated requests from Congressional committees, members of Congress, state regulators and journalists for information about specific drugs and companies.
“We want to make it so anyone can have the question about drug protections at their fingertips whenever they want,” Feldman said. “It’s designed to be easy and user-friendly, and to enhance public understanding about how competition may be limited rather than enhanced through the drug patent system.”
The database was created through a painstaking process of combing through 160,000 data points to examine every instance where a pharmaceutical company added a new drug patent or exclusivity.
“Most of it was done by hand,” Feldman said, “with multiple people reviewing it at every stage. And along the way we repeatedly made conservative choices. We erred on the side of underrepresenting the evergreen gain to be sure we were as fair and reasonable as possible.”
Among the 2,065 drugs covered in Evergreen Drug Patent Search, there are many examples of the evergreening strategy used by pharma to delay the entry of competition, especially generics, often for widely prescribed drugs, including those used to treat heartburn, chronic pain, and opioid addiction.
Nexium
Before Nexium, there was Prilosec, a popular drug to treat gastroesophageal reflux disease (GERD). But its patent exclusivity was due to expire in April 2001. In the late 1990s, with a precipitous drop in revenue looming, Prilosec’s manufacturer, AstraZeneca, decided to develop a replacement drug. Using “one-half of the Prilosec molecule — an isomer of it,” the result was Nexium, which received approval in February 2001.
Essentially an evergreened version of Prilosec, Nexium’s exclusivity was then extended by more than 15 years, as AstraZeneca received 97 protections stemming from 16 patents. These included revised dosages, compounds, and formulations. Feldman said that tinkering changes such as Nexium’s do not involve the substantial research and development required for a new drug, nor do they constitute true innovations, yet for a decade and a half, patients and taxpayers were forced to pay far more than was warranted for GERD relief. In fact, in 2016 — one year after patent exclusivity expired — Nexium still topped all drugs in Medicare Part D spending, totaling $1.06 billion.
Suboxone
Use of this combination of buprenorphine and naloxone for treating opioid addiction has exploded in the wake of the opioid epidemic. Since its approval, Suboxone’s manufacturer, Reckitt Benckiser (now operating as Indivior), extended its protection cliff eight times, gaining nearly two extra decades of exclusivity through early 2030.
The drug maker gained six patents for creating a film version of the drug — notably around the time protection was expiring for its tablet version. (The therapeutic benefits of the film and tablet are identical.) An earlier version of Suboxone also obtained an orphan drug designation, despite an opioid epidemic that has expanded Suboxone’s customer base to millions of potential customers. Suboxone generates more than $1 billion in annual revenue and ranks among the 40 top-selling drugs in the U.S.
Truvada
When Truvada, commonly referred to as PrEP, was approved in 2004, this HIV-prevention drug was a breakthrough. But 16 years later — and 14 years after its original exclusivity was to expire — it retains its monopoly status. Truvada’s manufacturer, Gilead, has received 15 patents and 120 protections since it came on the market, extending its exclusivity for more than 17 years, until July 3, 2024.
In countries where generic Truvada is available, PrEP costs $100 or less per month, compared to $1,600 to $2,000 in the U.S. As a result, Truvada is unaffordable to many people who need protection from HIV. Barred from access, they are left vulnerable to infection.
“We’re establishing a precedent that a pharmaceutical company can charge whatever it wants even as it allows an epidemic to continue, and the government refuses to intervene,” said James Krellenstein, co-founder of the group PrEP4All. “That should scare every American. If it’s HIV today, it will be another disease tomorrow.”
EpiPen
First approved in 1987, the EpiPen has saved the lives of countless numbers of people with deadly allergies. But it is protected from competition until 2025 — 38 years after its introduction — because its owner, Mylan, has filed five patents, four since 2010, all involving tweaks to the automatic injector. The actual medication used, epinephrine, has existed for more than a century — the innovation here is in the delivery device.
Because these small changes to the injector have maintained its monopoly for so long, the cost of an EpiPen package (containing two injectors) has risen from $94 when Mylan purchased the device to between $650 and $700 today. For many people, especially parents of children with severe reactions to common allergens like peanuts, EpiPen’s increasing price tag imposes an onerous financial burden.
What Can Be Done
As the Evergreen Drug Patent Search makes clear, the positive impact of Hatch-Waxman has been steadily and severely eroded by a regulatory system vulnerable to increasingly sophisticated forms of manipulation.
“You might say that the patent and regulatory system has been weaponized,” Feldman said. “When billions of dollars are at stake, there’s a lot of money available to look for ways to exploit the legal system. And companies have become adept at this, as our work has found.”
There are several key steps that Congress could take to restore the balance between innovation and competition that is the key to a successful prescription drug regulatory process. These may include:
- Imposing restrictions on the number of patents that prescription drug manufacturers can defend in court to discourage the use of anticompetitive patent thickets.
- Limiting the patentability of so-called secondary patents — which don’t improve the safety or efficacy of a drug — through patent and exclusivity reform.
- Reforming the 180-day generic exclusivity, which can currently be abused to block other competitive therapies.
“The Evergreen Drug Patent Search provides the publicly available, evidence-based foundation that defines the extent of the problem, and it can be used to develop policies that solve the problem of anti-competitive patent abuses,” said Kristi Martin, VP of Drug Pricing at Arnold Ventures.
“Our incentives have gotten out of whack,” Martin said. “The luxury of monopoly protection should only be provided to innovations that provide meaningful benefits in saving lives, curing illnesses, or improving the quality of people’s lives. It should not be provided to those gaming the system. If we can change that, we can save consumers, employers, and taxpayers many billions of dollars while increasing the incentives for pharmaceutical companies to achieve breakthroughs.”